
MedCity Pivot Podcast: Modernizing Prior Auth
In this episode, MedCity News' Arundhati Parmar chats with a pharmacy benefits leader and a virtual pharmacy operator about ways to modernize and scale prior authorization.

UnitedHealthcare is exempting rural providers from most prior authorization requirements.

Small practices play a critical role in healthcare delivery, but they cannot continue to absorb ever-increasing administrative demands without consequences.

Health insurers have reduced prior authorizations by 11% and are continuing reforms to streamline and speed up approvals, according to an announcement from AHIP and Blue Cross Blue Shield Association.

Technology alone won’t solve prior authorization. But refusing to adopt it guarantees the status quo: a system where insurers operate at machine speed, providers operate at human speed, and patients pay the price in delayed care.

With regulatory scrutiny intensifying and the demand for speed, compliance, and clarity growing, understanding the nuanced differences between AI approaches is essential for payers, providers, and patients alike.

More than 50 major insurers have pledged to streamline prior authorization starting in 2026, but providers remain cautiously optimistic and skeptical that the changes will truly reduce burden or delays in care.

Here are three things providers should consider when it comes to Medicare.

Take our quiz and learn more about perspectives on AI and RCM in healthcare.

Health systems should take the lead in fixing the broken prior authorization process, said Jeff Balser, CEO of Vanderbilt University Medical Center, during a recent conference. He highlighted AI, better workflows and centralized support as ways to reduce delays.

Thirteen House Democrats introduced eight bills to rein in Medicare Advantage and bolster traditional Medicare.

AI and advanced analytics can help organizations move beyond incremental fixes, streamlining access and improving patient experience, without overburdening staff or budgets.

Guideline directed care pathways are a way to shift from transactional PA, where each service requires separate approval, to an episode-of-care model.

Cohere Health and Microsoft have teamed up to use ambient listening and AI to simplify and speed up the prior authorization process, part of a broader industry shift toward reducing paperwork and improving care at the point of service.

Develop Health's Series A funding round was led by Wing Venture Capital, and included participation from Afore Capital, J Ventures and South Park Commons.
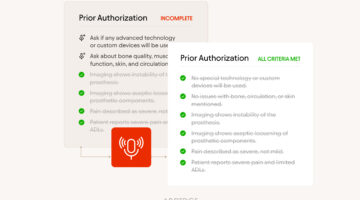
Highmark Health recently announced a partnership with AI technology company Abridge to deploy its ambient clinical documentation platform across Allegheny Health Network and co-develop a new prior authorization solution.